I remember how shocked I was when I logged my first score of 1. I was at my parent’s house, having a home cooked meal. A usual Sunday dinner, we had ground beef kabob with basmati rice. Grilled over charcoal, and with only a few simple ingredients, the kabob tastes delicious and has a light smokiness to it you can’t get from a gas grill or oven. The rice, topped with saffron, was a perfect compliment, soaking all the juices and fat from the kabob. Supposedly, my ancestors consumed this classic meal for generations.
According to the continuous glucose monitor (CGM) attached to my arm though, the meal wrecked my glucose levels. On a 1-10 scale, the meal’s score of 1 was the lowest and worst possible score.
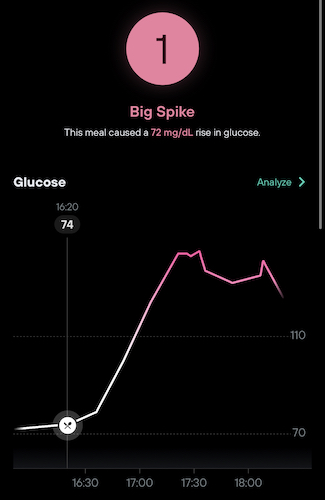
It’s no surprise that you should consume rice in small quantities. But it was shocking to see how, for the next two hours, my glucose level stayed high as my body grappled with the influx of sugar and carbs.
As I continued to wear the CGM, I was surprised over and over again by the glucose response for my favorite meals.
It was an emotional rollercoaster.
That garden vegetarian sandwich at one of my favorite local restaurants? A dismal 2. Bagel with smoked salmon and cream cheese? Not as bad as I thought: a 6. An innocent peanut butter jelly sandwich? A 4.
Your glucose levels matter
If wearable technologies have allowed us to see a blurry, pixelated image of how healthy we are, CGMs will make that image sharper than ever before.
Step counters, heart rate trackers, and sleep trackers: we use wearables and smart watches to understand how active we are, how restful our sleep is, and how our heart rate and heart rate variability changes during the day and during exercise. But we need more data about what’s happening inside us.
For diabetics, continuous glucose monitors were introduced 20 years ago as an alternative to pricking your finger. With a glucose sensor applied to your arm, you can see your blood glucose level through a reader or your smartphone. By having access to this data, diabetics can adjust their diet and use insulin as needed.
Your glucose levels and your body’s insulin response can have profound effects on your health. From physician Peter Attia:
Higher glucose variability and higher (and more) peak glucose levels are each independently associated with accelerated onset of disease and death, even in nondiabetics…higher glucose variability in nondiabetics is associated with an increased risk of cardiovascular disease, Alzheimer’s disease, frailty, cardiovascular death, cancer death, and death from any cause compared to lower glucose variability.
I’ve worn a CGM on and off for the last year. Levels, a company that offers a CGM paired with a mobile application, gets you the prescription you need for a CGM and ships it to your door. As you eat throughout the day, you log your foods, and Levels assigns a 1-10 score. 1 means that the meal caused a big spike in glucose, 10 means that your body had a stable response. You want more 10s than 1s.
As CGMs become accessible to the rest of us, continuous glucose monitors will unlock a new stream of data for non-diabetics: our body’s unique glucose response to different foods. With CGMs, we can have real-time feedback on the foods we eat. We can make small changes to improve our metabolic health.
A world where everyone has a CGM
This summer, while overseas in the Netherlands, I was sitting outside with my five year old son at a restaurant. Nearby, an older Dutch woman pulled out a cigarette. My son looked confused and whispered to me:
“What is that thing that she was holding but she also blew it out? Why did she do that?”
The concept of a cigarette was foreign to him.
What will the world look like when anyone can access a CGM for little or no cost? Will we consider giving a kid candy as bad as we now think of giving a kid a cigarette?
Seeing your body’s glucose response over time will offer a clearer view on the impact of food than any traditional metrics we have used in the past. Our rubric for food will change. We’ve been seeing food through the lens of macros, calories, and nutritional content. Glucose variability offers yet another data point.
Food companies can no longer hide behind labels and marketing. Organic cane sugar is still…sugar. Companies will need to re-engineer their foods to appeal to a more sugar conscious population. Armed with more information than ever before, we won’t need to jump from one diet to another. Instead, we can make small changes to what we eat to reduce glucose variability.
Conducting your own experiments with a CGM
For the enthusiast, wearing a CGM opens up a whole world of experimentation. While far from a scientific study, having a CGM has given me actionable n=1 data:
- How is your glucose response to the same food if you eat it in the morning instead of the afternoon? In my case, I see less of a spike in the morning.
- What about changing the order in which you eat your meal? Protein before carbs helps reduce spikes.
- What happens when you reheat food? Starches like rice cause less of a spike when reheated.
Other people wearing CGMs have posted their experiments online. From taking a tablespoon of apple cider vinegar to lower glucose spikes to seeing how stress impacts glucose levels, there are endless opportunities to learn about how your body responds to food and the environment.
Will having a CGM change how you eat?
It’s up to us to use CGMs in a meaningful way to drive our behavior. We all know people that have expensive gadgets to measure every aspect of what they do, but they’re still out of shape and eating poorly.
Like throwing your fitness tracker into the dryer to beat your coworkers in a step tracking challenge, you can game a CGM. If I sit on my couch, chug whiskey and eat bacon all day, I won’t see a spike in glucose. My consumption would be low carb. But that doesn’t mean that I’m being healthy in what I’m consuming.
Will getting a better understanding of how your body reacts (or doesn’t) to different foods change what you eat? Possibly. For me, wearing a CGM has had lasting behavioral effects: I now think twice before consuming processed foods and have made efforts to avoid glucose-spiking meals in the evening. I wear a CGM less frequently now. When I do I use it as an accountability tool and to continue to test how I can reduce spikes in meals that I enjoy.
Glucose levels and how variable they are isn’t the only metric that matters. If your body is able to quickly react and provide the insulin needed, a spike in glucose might not be that bad. But combined with other biomarkers, we now have a more holistic picture of our health than ever before. As continuous health monitoring becomes a reality, we can imagine a future where we eliminate diseases of diet and save on healthcare costs, making us all stronger and healthier.